A bee sting is a small but painful wound caused when an insect’s stinger pierces the skin and injects venom. Most people will feel brief pain, mild swelling, and local redness. Honey bees often leave a barbed stinger behind, which can increase venom exposure if not removed quickly.
This short guide explains simple care steps that limit venom spread, ease pain, and promote healing for most people at home. You will learn safe stinger removal, gentle skin cleansing, and ways to protect the affected body area.
Serious symptoms — such as trouble breathing, dizziness, or widespread hives — require calling 911 or a trip to the ER. About 5% of people in the United States are allergic to insect stings, so knowing warning signs can be lifesaving.
Key Takeaways
- Remove the stinger quickly and clean the area to reduce venom on the skin.
- Use cold compresses and over-the-counter options to relieve pain and swelling.
- Watch for severe symptoms; seek emergency care for breathing issues or fainting.
- Single and multiple stings differ in risk; more venom may mean more care.
- Prevention in gardens and parks lowers the chance of future stings.
- Most cases can be managed at home, but know when to escalate to medical care.
Understanding bee stings, symptoms, and when they’re common
Outdoor encounters with flying insects often lead to sudden pain, redness, and swelling where the skin was pierced.
Types of bees matter. Honey bees are slender and tan-yellow/black and often leave a stinger behind. Bumble bees are larger and furry, while carpenter bees look shiny with yellow hairs on the thorax. Knowing this helps predict whether a stinger may remain in the skin.
Bees are active in warm times of the year and near flowers, so people face the highest risk in gardens, parks, and around flowering trees. Most local reactions include sharp pain, localized swelling, itching, and warmth at the area.
Act quickly when a stung bee might have left a stinger: note the time, remove any visible stinger, and cleanse gently with soap and water if the skin is unbroken. Monitor symptoms for 24–48 hours, and watch for signs that the reaction is spreading beyond the bite site.
- About 5% of people in the U.S. have an allergy to insect stings, so know warning signs.
- If you want more detail on symptoms and when to seek care, see the official guidance on bee stings.
Bee sting treatment: step-by-step instructions for quick relief
Start with hands-on care right away — quick removal and cooling reduce local symptoms effectively.
Remove the stinger promptly to limit venom exposure
Act quickly. If a barbed stinger is visible, scrape or pinch it out without delay. Promptly removing the stinger limits extra venom and can shorten symptoms after a bee sting.
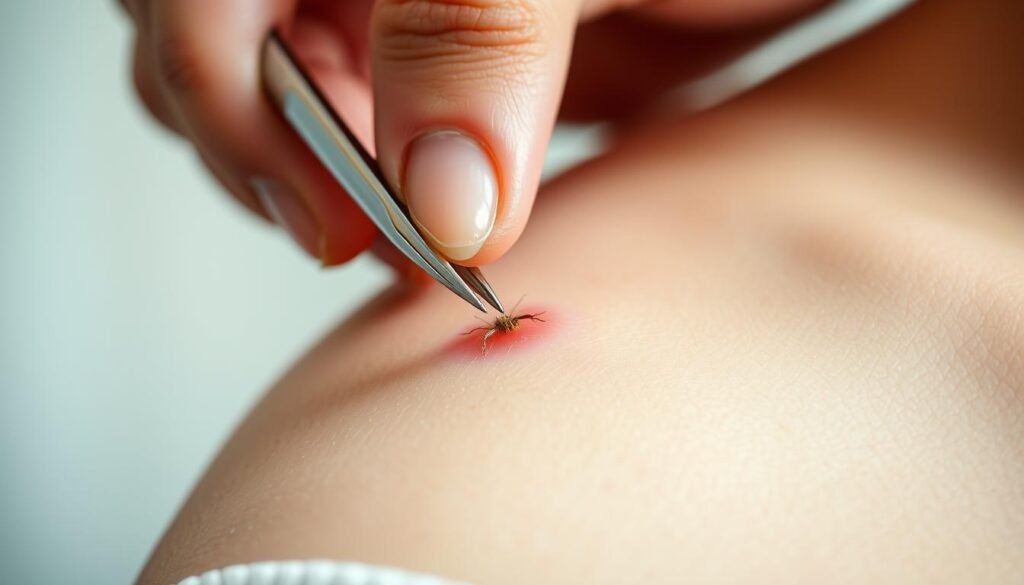
Clean the affected area with soap and water
After removal, wash the site gently with mild soap and cool water to lower infection risk. Keep the skin clean and pat dry; avoid rubbing or probing the area.
Apply a cold pack to reduce swelling and relieve pain
Use a wrapped ice pack for 10–15 minutes, then pause and repeat as needed. Icing helps reduce swelling and can quickly relieve pain at the skin site.
Supportive care: oral pain relievers and anti-itch strategies
For home care, consider an over-the-counter pain reliever per label instructions and an oral antihistamine for itching if appropriate. Keep the affected area elevated on a limb to help reduce swelling.
- Do not squeeze the site or delay remove stinger while searching for a tool — prompt action matters.
- Monitor for growing redness, expanding swelling, or systemic signs and seek emergency care if they appear.
- If you have a known allergy, use your epinephrine auto-injector and get emergency help right away.
- Some people apply a small amount of honey as a soothing, nonclinical option, but this should not replace core care steps.
Typical reactions versus concerning symptoms after a sting
Most reactions after an insect bite stay limited to the nearby skin and ease with basic care.
Normal local reactions: pain, redness, itching, and swelling
Common signs include sharp pain at the site, redness, mild swelling, and itching of the surrounding skin.
Pain usually begins to fade within about an hour. Swelling may persist for several days and often peaks within 24–48 hours.
Warmth and tenderness are normal, but the area should slowly improve with cleaning, icing, and rest.
When symptoms spread beyond the sting site
If redness or swelling rapidly expands, or if hives appear away from the area, treat this as a warning sign.
Seek urgent care when breathing difficulty, dizziness, or signs of anaphylaxis appear — these suggest an allergic reaction that needs immediate evaluation.
Also check for a retained stinger; removal can help the reaction subside. When in doubt, get prompt assessment.
| Reaction type | Typical timeline | Action |
|---|---|---|
| Local mild | Pain improves in ~1 hour; swelling 1–7 days | Clean, ice, monitor |
| Enlarged local | Swelling peaks 24–48 hours | Oral antihistamine, medical advice if worsens |
| Systemic / allergic | Rapid onset after exposure | Emergency care for anaphylaxis or widespread hives |
Recognizing an allergic reaction and urgent treatment steps
If someone quickly develops hives, lightheadedness, or throat tightness after a sting, treat it as a medical emergency. Early recognition speeds lifesaving care.
Signs that require immediate action
Anaphylaxis can include widespread hives, difficulty breathing, dizziness, or swelling of the lips, tongue, or throat. Any of these signs needs instant attention.
Use of epinephrine and calling 911
If you have a prescribed epinephrine auto‑injector, use it at the first sign of anaphylaxis and call 911 immediately. After injection, lie down with legs elevated if possible and wait for emergency responders.
When multiple or airway stings need emergency evaluation
More than 10 stings at one time raises risk even in people without prior allergy. Stings inside the mouth, nose, or throat may cause rapid airway swelling and demand urgent care.
- Antihistamines may ease itching or hives but do not replace epinephrine for anaphylaxis.
- Seek monitored care after any epinephrine use—symptoms can recur and further treatment may be needed.
- Discuss long‑term prevention and allergy evaluation with a clinician after an emergency.
For additional emergency care guidance and follow‑up recommendations, consult a medical provider promptly.
Bee vs. wasp, hornet, and yellow jacket stings: what changes in care
Different insects deliver venom differently, so recognizing the type matters for immediate action. A quick visual check helps you decide whether to search the skin for a retained stinger and how closely to watch symptoms.
Single sting versus multiple stings: stinger type and risks
Single versus multiple punctures and when to be more concerned
Honey bees often leave a barbed stinger behind. That stinger can keep releasing venom until removed, so prompt removal is key.
Wasps, yellow jackets, and hornets have smooth stingers and can sting many times. Multiple stings raise the total venom load and increase the chance of worse symptoms.
How to identify bees and wasps and why it matters
Bees tend to look furry and rounder. Wasps appear shiny with a narrow waist and little hair. Bumble and carpenter bees show distinct size and coloring.
If you cannot tell, follow basic care: cleanse the skin, apply cold, and monitor for spreading pain, swelling, or itching. Seek care sooner after multiple punctures or rapid symptom growth.
| Insect | Stinger | Risk after one encounter | Key first step |
|---|---|---|---|
| Honey bee | Barbed (often retained) | Venom continues until stinger removed | Scrape out stinger, clean, ice |
| Wasp / yellow jacket | Smooth (multiple stings possible) | Higher venom if stung many times | Count sites, clean, monitor closely |
| Hornet | Smooth, can sting repeatedly | More painful; possible larger swelling | Cold pack, watch for systemic signs |
Home care options to relieve pain and reduce swelling
Immediate home care helps limit swelling and speeds comfort at the affected skin site. Rest the limb or area and keep the site clean with cool water. Use a wrapped cold pack for 10–15 minutes at a time to reduce swelling and relieve pain.
Many people try simple remedies. A baking soda and water paste or a dab of unseasoned meat tenderizer mixed with water may ease local discomfort, though evidence is limited. Some apply a thin layer of honey; darker varieties like buckwheat honey have added antioxidants but should complement standard care.
Other options that can soothe itching at the affected area include bentonite clay, calamine-like lotions, or repeated cool compresses. An oral antihistamine can help with itching, but it will not prevent a severe allergic reaction.
- Elevate the limb when possible and reassess pain and swelling regularly.
- Keep the skin dry between cold treatments and avoid scratching to limit redness and infection.
- Stay hydrated and avoid heavy activity that stresses the area.
Seek urgent care if more than 10 punctures occurred, or if the mouth, nose, or throat is involved. For additional home remedy context see home remedies for bee stings.
Conclusion
Quick action, simple steps, and calm judgment often prevent a minor event from becoming an emergency.
Promptly remove a visible stinger to limit further venom at the site, clean gently, and apply cold. Most cases improve with basic home care and close observation.
If breathing problems, dizziness, or widening symptoms occur, call 911 immediately and get emergency attention. For an allergic reaction, use epinephrine if prescribed and seek medical care without delay.
Remember that honey bees commonly leave a stinger while wasps do not. Keep a seasonal plan for health and review it with your clinician if you have prior severe reactions.
FAQ
What are the most effective options for immediate relief after a bee sting?
For quick relief, remove any visible stinger, wash the area with soap and water, apply a cold pack for 10–15 minutes to reduce swelling and pain, and take an oral pain reliever like ibuprofen or acetaminophen if needed. An oral antihistamine such as cetirizine or diphenhydramine can help control itching and minor swelling. Monitor the site for worsening symptoms.
How do I know if a reaction is normal or needs medical attention?
A normal local reaction includes pain, redness, mild swelling, and itching confined to the area. Seek medical care if swelling increases over hours, redness spreads, fever develops, or if you notice signs of infection (increasing warmth, pus). If symptoms extend beyond the immediate area or you experience systemic signs, get urgent help.
What are signs of a severe allergic reaction I should watch for?
Watch for hives, widespread swelling, difficulty breathing or swallowing, wheezing, dizziness, fainting, fast heartbeat, or sudden drop in blood pressure. These symptoms indicate anaphylaxis and require immediate use of an epinephrine auto-injector if available and calling 911 right away.
How should I remove a stinger to limit venom exposure?
Scrape the stinger off quickly with a flat edge like a credit card or use tweezers if necessary. Avoid squeezing the venom sac, which can push more venom into the skin. Clean the area after removal to lower infection risk.
Are home remedies such as honey, baking soda, or ice effective?
Cold compresses and clean water are reliable first-line measures. A paste of baking soda may help neutralize some venom for alkaline-sensitive insects, and honey has antimicrobial properties but limited evidence for reducing pain. Avoid unproven or irritating substances that can worsen skin reaction.
When should I use an epinephrine auto-injector and then call emergency services?
Use epinephrine immediately if you suspect anaphylaxis—difficulty breathing, throat tightness, widespread hives, or fainting. After administering epinephrine, call 911 because symptoms can recur or worsen and further medical care is necessary. If you don’t have an auto-injector and signs of anaphylaxis appear, call 911 immediately.
Does treatment differ between stings from bees, wasps, hornets, or yellow jackets?
General first aid is the same: remove any stinger, clean the area, cold compresses, and monitor. Wasps and hornets typically don’t leave a stinger behind, and some species inject more venom or sting repeatedly, raising the risk with multiple stings. Identify the insect if possible to inform medical staff, especially after multiple stings.
What should I do if someone receives multiple stings or is stung in the mouth, nose, or throat?
Multiple stings or stings to airway areas increase the risk of severe swelling and systemic toxicity. Call 911 immediately. Keep the person calm and still, watch breathing, and give epinephrine if signs of anaphylaxis appear. Rapid transport to emergency care is essential.
How long do typical local reactions last, and when should I see a doctor for persistent symptoms?
Local pain and swelling usually peak within 24–48 hours and improve over several days. See a doctor if redness or swelling worsens after 48 hours, symptoms persist beyond a week, you develop fever, or the area shows signs of infection.
Which over-the-counter medications help with pain and itching?
Oral NSAIDs (ibuprofen) or acetaminophen help pain. Oral antihistamines like cetirizine, loratadine, or diphenhydramine reduce itching and allergic symptoms. Topical hydrocortisone can ease inflammation and itching at the site. Follow dosing instructions and consult a clinician for children, pregnant people, or those with chronic conditions.
Can someone become allergic after previous mild reactions?
Yes. Sensitization can change over time; a person with past mild reactions can develop more severe responses later. If you have had increasing reactions or are at risk, talk to an allergist about testing and a possible epinephrine auto-injector prescription.
How can I prevent stings when spending time outdoors?
Wear long sleeves and pants, avoid bright floral prints and strong fragrances, keep food and drinks covered, and use insect screens when possible. Be cautious around nests and flowering plants. If you have known severe allergy, carry an epinephrine auto-injector and wear medical identification.
Are children at greater risk for complications from multiple stings?
Children can be more vulnerable to systemic effects from multiple stings because of smaller body mass. Seek medical care promptly after multiple stings or any signs of breathing trouble, swelling of the face or throat, vomiting, or fainting.
Should I see an allergist after an emergency sting?
Yes. After anaphylaxis or a severe systemic reaction, follow up with an allergist to confirm the allergy, discuss epinephrine use, and consider immunotherapy if appropriate. The specialist can create an action plan to reduce future risk.